We use cookies to enhance your experience and to comply with data protection regulations. By clicking "Accept", you agree to our use of cookies. Read more.
Ophthalmologist & Facial Aesthetics


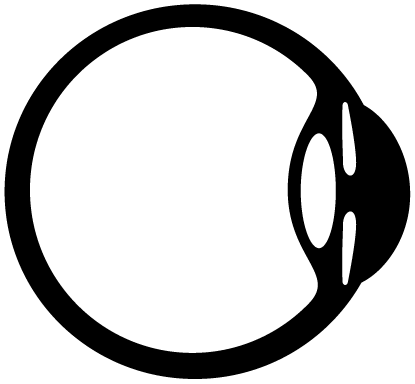

Keratoconus is a condition in which the cornea (transparent layer in front of the coloured iris) becomes increasingly thin, irregular and protrudes out. It is derived from the Greek words ‘Keras’ (meaning Cornea) & ‘Konos’ (meaning Cone). If Keratoconus is not adequately treated, the vision naturally evolves from slightly blurred vision (correctable with glasses/contact lenses), to significant vision loss (requiring surgical corneal implants or transplants).
There are 4 main risk factors for Keratoconus
▪ Eye rubbing – there is a very high risk in people who frequently rub their eyes (a common trait with allergic conjunctivitis, eczema, hay-fever, asthma).
▪ Genetic factors – a person is 15 times more likely to develop keratoconus if they have a parent, sibling or child with keratoconus.
▪ Hormonal & Environmental factors – research has shown links between hormonal regulation and environmental effects on keratoconus development.


Keratoconus always involves both eyes, but to different degrees. Symptoms include:





There are a multitude of effective keratoconus treatments available.
A customised treatment regimen will be designed for your level of keratoconus after a comprehensive consultation and specialised tests with Dr. Djan.
The treatment armamentarium includes:





CXL is a painless procedure that aims to reinforce & strengthen the cornea, preventing further thinning. It uses the power of Riboflavin (Vitamin B2) and Ultra-Violet light (UV-A) to form rigorous bonds within the cornea.
A stronger, fortified cornea that resists further keratoconus thinning (success rate 95-99%). Successful CXL treatment prevents the the natural progression of keratoconus that would otherwise lead to corneal hydrops (cloudy scarring) and the need for a corneal transplant.
CXL is a painless procedure performed with anaesthetic (numbing) eyedrops and light sedation that lasts approximately 45 minutes in a sterile facility. Firstly, numbing anaesthetic eyedrops are placed onto the eye while you lay on your back. Next, the surface layer (epithelium) is gently exfoliated. This allows the applied Riboflavin (Vitamin B2) eyedrops access to soak evenly through the cornea. Medical-grade UV-A light is then directed towards the cornea to activate the chemical reaction (photo-polymerisation) responsible for fortifying the cornea. Antibiotic eyedrops are then instilled and a protective contact lens is placed onto the eye for about 3-5 days.
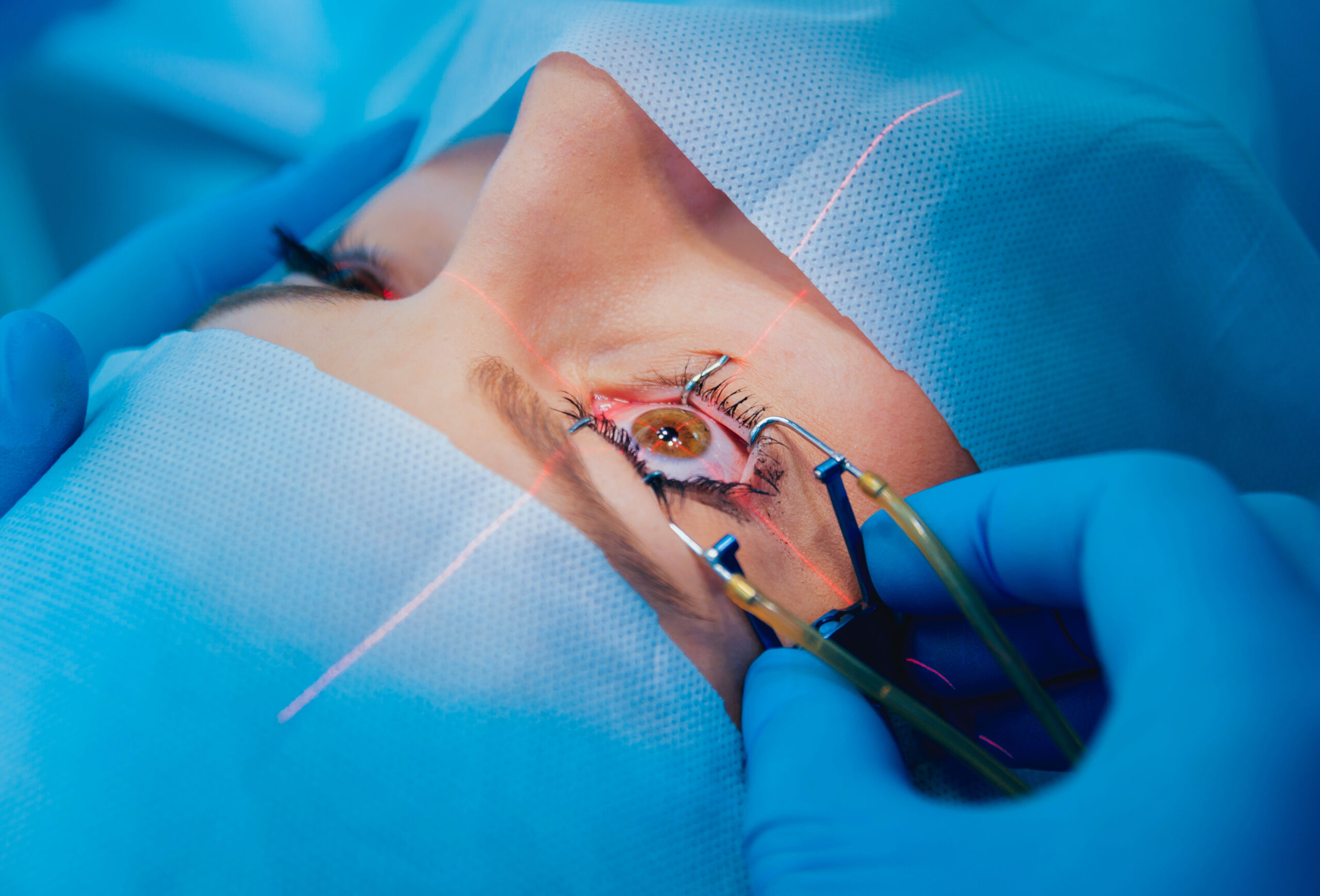
Most people find they are able to return to their usual level of activities approximately 1 week after CXL. Prescription eyedrops use is continued for weeks after the procedure to combat any eye inflammation (characterised by light sensitivity/grittiness/blurred vision).
Although CXL is a very safe procedure, all medical procedures have inherent risks. CXL is painless, however, some patients do encounter varying degrees eye discomfort/tenderness and light sensitivity for the the first 24 hours after the procedure. Other rare risks includes an eye infection. The eyedrops Dr. Djan prescribes are aimed at mitigating any of the above risks. In a few patients (1-5%), the CXL procedure may need to be repeated if the keratoconus thinning continues to progress.
No. CXL is a highly effective (95-99%) keratoconus treatment aimed at stopping the corneal thinning process and preventing further loss of vision. It is designed to stabilise the eye, NOT to improve your current vision and therefore spectacles/contact lenses will still be required thereafter. Keratoconus is a lifelong condition that requires monitoring.
Corneal implants (Intrastromal Ring Segments such as ISCRS or CAIRS) are transparent, microscopic, semi-circular implants that provide much needed structural support to the weakened keratoconus cornea, analogous to the function of dental braces. Their small size and transparent nature means that they are invisible to the patient and any observer.




Corneal implants are performed with anaesthesia eyedrops and light sedation. A laser creates a microscopic tunnel inside the cornea with the perfect dimensions to house the implant.
The implant is manually glided into the tunnel. One or two implants may be implanted depending on the configuration of your individual cornea.
No sutures are used, antibiotic drops are then instilled & a contact lens is placed onto the eye for a day or two as it heals. Corneal implant surgery my be combined with CXL in certain instances for a more robust result.
Corneal implant surgery is a day procedure and most people find that they are able to return to their usual level of activities approximately 5-7 days afterwards. Mild eye inflammation (characterised by light sensitivity/grittiness/blurred vision) is uncommon, but may be present for a few hours thereafter. Dr. Djan prescribes an anti-inflammatory eye drop in such cases which resolves shortly thereafter.
Corneal implant surgery is a very safe procedure, however, all medical procedures have inherent risks.
Risks are uncommon and may include: 


Indirectly, yes. Corneal implant improves the quality of vision in conjunction with your contact lenses. The primary function of corneal implants is to create a stable scaffold for your irregular keratoconus cornea.
This is particularly useful in people who are contact lens intolerant:
(1) People who have functional vision with contact lenses, but now experience extreme discomfort wearing them or struggle to keep their contact lenses on beyond a few hours at a time
(2) People who are new to contact lenses, but don’t have a suitable corneal shape to allow contact lens fitting.
A stable cornea is then able to accommodate contact lenses better to vastly improve vision quality.

Scleral contact lenses are custom-made to an individuals unique eye shape using specialised digital & imaging equipment, different to that required for regular soft contact lenses. They are larger and more stable than soft contact lenses and fit over both the cornea and part of the sclera (white part of the eye). Anyone interested in having crisp, clear vision may be a candidate for SCLs.
These lenses are however, extremely advantageous in providing sharper quality vision and a comfortable fit in patients with:







Yes. Don’t allow costs to limit your eye health and aesthetic appearance. Tailored Finance options are available to suit your individual needs.